 |
 |
| Tuberc Respir Dis > Volume 85(2); 2022 > Article |
|
Abstract
Background
Methods
Results
Conclusion
Notes
Authors’ Contributions
Conceptualization: Hong Y, Hong JY, Park J. Methodology: Hong Y, Hong JY, Park J. Formal analysis: Hong Y, Hong JY, Park J. Data curation: Hong Y, Hong JY, Park J. Software: Park J. Investigation: Hong Y, Hong JY, Park J. Writing - original draft preparation: Hong Y, Park J. Writing - review and editing: Hong Y, Kim WJ, Jeong Y, Hong JY, Park J. Approval of final manuscript: all authors.
Funding
This study was supported by a grant (NRF 2020R1A2C 1011455) of the National Research Foundation (NRF) funded by the Korean Government and a grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HI21C1074).
Fig. 1.
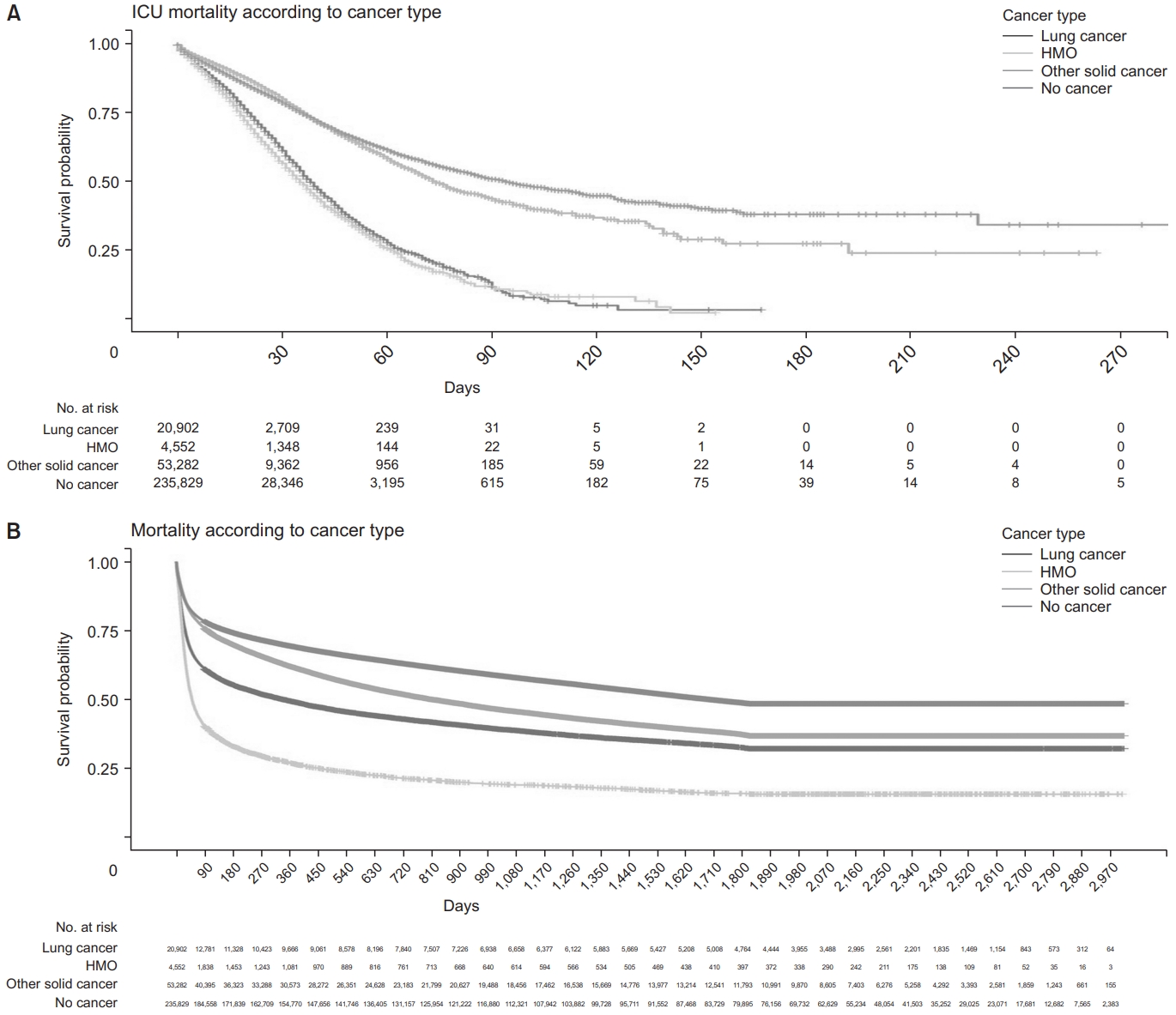
Fig. 2.
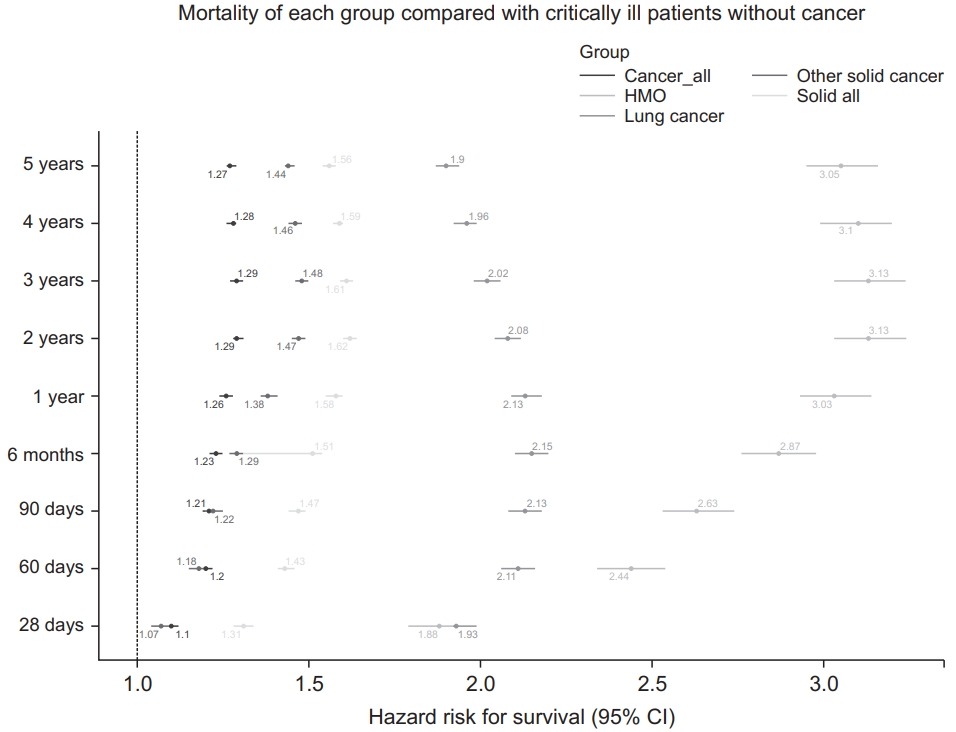
Table 1.
Table 2.
REFERENCES
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 9,222 View
- 2,846 Download
- ORCID iDs
-
Yoonki Hong

https://orcid.org/0000-0002-1607-6777Jinkyeong Park

https://orcid.org/0000-0002-8833-9062 - Funding Information
-
National Research Foundation of Korea
https://doi.org/10.13039/501100003725
2020R1A2C1011455Korea Health Industry Development Institute
https://doi.org/10.13039/501100003710Ministry of Health and Welfare
https://doi.org/10.13039/501100003625
HI21C1074 - Related articles
-
Bacteriologic Analysis of Expectorated Sputum in Patient with Bronchiectasis.2009 December;67(6)


 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Print
Print Download Citation
Download Citation



