Exhaled Nitric Oxide in Patients with Stable Chronic Obstructive Pulmonary Disease: Clinical Implications of the Use of Inhaled Corticosteroids
Article information
Abstract
Background
Fractional exhaled nitric oxide (FeNO) is regarded as a potential biomarker for identifying eosinophilic inflammation. We aimed to evaluate the clinical implication of FeNO and its influence on inhaled corticosteroids (ICS) prescription rate in Korean chronic obstructive pulmonary disease (COPD) patients.
Methods
FeNO level and its association with clinical features were analyzed. Changes in the prescription rate of ICS before and after FeNO measurement were identified.
Results
A total of 160 COPD patients were divided into increased (≥25 parts per billion [ppb], n=74) and normal (<25 ppb, n=86) FeNO groups according to the recommendations from the American Thoracic Society. Compared with the normal FeNO group, the adjusted odds ratio for having history of asthma without wheezing and with wheezing in the increased FeNO group were 2.96 (95% confidence interval [CI], 1.40–6.29) and 4.24 (95% CI, 1.37–13.08), respectively. Only 21 out of 74 patients (28.4%) with increased FeNO prescribed ICS-containing inhaler and 18 of 86 patients (20.9%) with normal FeNO were given ICS-containing inhaler. Previous exacerbation, asthma, and wheezing were the major factors to maintain ICS at normal FeNO level and not to initiate ICS at increased FeNO level.
Conclusion
Increased FeNO was associated with the history of asthma irrespective of wheezing. However, FeNO seemed to play a subsidiary role in the use of ICS-containing inhalers in real-world clinics, which was determined with prior exacerbation and clinical features suggesting Th2 inflammation.
Introduction
Chronic obstructive pulmonary disease (COPD) is a progressive inflammatory airway disease characterized by persistent airflow limitation1. For patients with stable symptomatic COPD, inhaled bronchodilators are the mainstay of treatment to control symptoms1. Although the use of inhaled corticosteroids (ICS) is recommended only for COPD patients who experience frequent exacerbations, discrepancies have often been reported among recommendations and actual clinical practice, where ICS, especially in combination with a long-acting beta-agonist, are widely used in the management of COPD patients234. The overuse of ICS as maintenance therapy clearly raises a concern due to the increased risk for pneumonia and adverse effects of long-term use of ICS567. Thus, it is imperative to investigate clinical features and indicators to predict a favorable ICS response in patients with COPD.
Neutrophilic airway inflammation is a prominent feature in most COPD patients and related to the degree of airflow limitation8. However, increased eosinophilic inflammation has been reported in a subset of patients with COPD, and approximately 20% of smokers with COPD have a Th2-high signature91011. These patients exhibit a greater response to short-term oral and ICS treatment1213; however, sputum specimens have limited value in clinical applications because of contamination risk and difficulty in collection. Accordingly, blood eosinophil count has emerged as an alternative biomarker to predict which subset of patients will benefit from steroid treatment141516. Although blood eosinophil count over 300 cells/µL is regarded as threshold for predicting high likelihood of benefit with ICS1718, variability on serial blood eosinophil counts examination may be problematic1920.
Another simple and noninvasive measurement reflecting eosinophilic airway inflammation is fractional exhaled nitric oxide (FeNO). In several studies, FeNO has demonstrated a correlation with eosinophilic airway inflammation2122 and a recent study reported that FeNO measurement is useful in patients with non-specific respiratory symptoms to predict response to ICS23. Despite the increasing attention devoted to FeNO in clinics, there are limited data regarding clinical characteristics related to eosinophilic airway inflammation and high FeNO levels in patients with stable COPD. Moreover, research investigating clinician behavior, such as addition or withdrawal of ICS based on FeNO value, is not available. Thus, we aimed to investigate the relationship between history of asthma and/or wheezing and increased FeNO levels in patients with stable COPD. We further assessed whether FeNO values affect ICS prescription in a real-world setting.
Materials and Methods
1. Patients
The Korea COPD Subgroup Registry and Subtype Research (KOCOSS) (registered with ClinicalTrial.gov identifier NCT02800499) is an ongoing, multi-center, prospective observational cohort study, launched in December 2011, with 48 centers in Korea participating. Details of the KOCOSS study have been previously published24. Participants aged ≥40 years and post-bronchodilator forced expiratory volume in 1 second (FEV1)/forced vital capacity <70% were included in the COPD cohort. In 2016, the KOCOSS protocol was updated to include FeNO measurement, and 160 patients from the KOCOSS cohort, whose FeNO was measured during stable period of COPD was identified from the KOCOSS cohort. All study procedures were performed in accordance with the Declaration of Helsinki and relevant guidelines, and informed consent was obtained from all participants before enrollment. The study protocol was approved by the Institutional Review Board of Samsung Medical Center (IRB No. 2018-05-055-001).
2. Clinical measurements
At initial evaluation, demographic and clinical data, including, age, sex, and body mass index, smoking status, history of physician-diagnosed asthma, subjective wheezing, modified Medical Research Council dyspnea scale, self-perceived quality of life status, assessed using the COPD assessment test, were collected by physicians or trained nurses using electronic case-report forms. A blood sample was collected, and blood eosinophil and total IgE were quantified and verified.
Spirometry was performed using standardized equipment according to the recommendations of the American Thoracic Society (ATS) and the European Respiratory Society (ERS) guidelines25. Based on the ATS/ERS guidelines, spirometry was performed before and after a 15-minute delay of the inhalation of 2 puffs of salbutamol to assess bronchodilator response (BDR). The predicted percentage values for the results of spirometry were calculated from the equation developed in Korean populations26.
3. Measurement of FeNO
According to the ATS guideline27, FeNO levels were measured by asking patients to inhale a maximum amount of air outside the valve and then exhale into the valve which in turn was connected to a chemiluminescent NO analyzer (NIOX MINO, Aerocrine AB, Solna, Sweden) or NObreath (Bedfont Scientific, Maidstone, UK), depending on the device each hospital was equipped with. FeNO levels were measured twice to verify reproducibility and validity; the mean value of FeNO was subsequently calculated. A FeNO <25 parts per billion (ppb) was regarded as normal and ≥25 ppb as increased, in accordance with the recommendations from the ATS27.
4. Statistical analysis
Data are expressed as mean±standard deviation, or absolute number with percentages unless otherwise indicated. To analyze baseline characteristics, the Pearson's chi-squared test was used for categorical variables, while the Student's t-test or Fisher's exact test was used for continuous variables. To assess the correlation between blood eosinophil and FeNO values, Pearson correlation analysis was performed. The degree of agreement between two values is expressed as the correlation coefficient, r, for which a positive value indicates a positive correlation and the higher the value, the stronger the correlation. Thus, the clinical characteristics of COPD patients according to FeNO level were analyzed using logistic regression analysis based on a FeNO value of 25 ppb. The multivariable logistic regression analyses were adjusted for covariates such as age, sex, smoking status and FEV1 <50% predicted.
All analyses were two-sided, and a p-value of <0.05 was considered to be statistically significant. All analyses were performed using STATA version 13.1 (StataCorp., College Station, TX, USA).
Results
1. Patient characteristics
The mean age of the 160 COPD patients was 70.5 years and most (n=150, 93.9%) were male and current or ex-smokers (n=153, 95.6%). Mean FeNO level was 27.1±17.3 ppb and mean eosinophil count was 190.8±161.9 cells/mL (Table 1).
Using cut-off value of 25 ppb, 74 patients (46.3%) had increased FeNO. Those patients were more likely to have a history of asthma (37.8% vs. 19.8%, p=0.011) or a history of asthma with accompanied wheezing (18.9% vs. 7.0%, p=0.023) compared with those with normal FeNO levels.
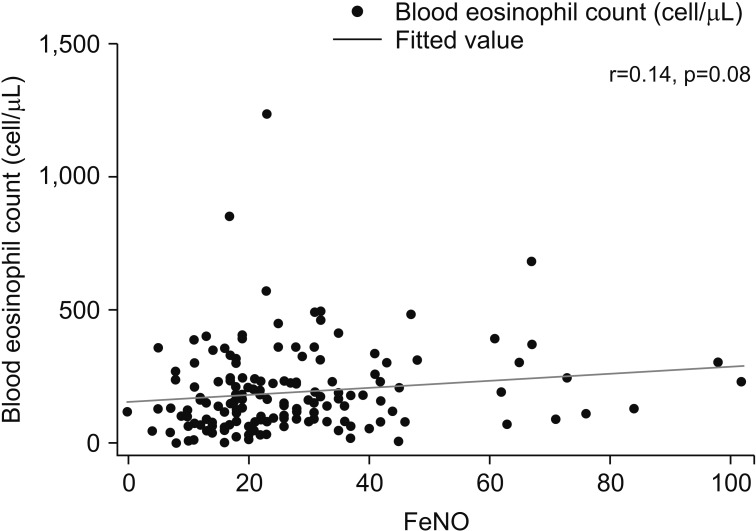
The severity of respiratory symptoms, self-perceived disease-specific quality of life status, and lung function were not significantly different between the two groups. Although patients with increased FeNO level demonstrated a positive BDR more frequently, the difference was not statistically significant (Table 2). Blood eosinophil count was higher in the increased FeNO group than in those with normal FeNO level without statistical significance (207.2 cells/mL vs. 176.6 cells/mL, p=0.242) (Table 2). The level of FeNO and blood eosinophil count demonstrated a positive but no significant correlation (Figure 1).
2. Association between increased FeNO level and history of asthma and wheezing
To investigate the association between increased FeNO and history of asthma with or without subjective wheezing, patients were categorized in to three groups according to the presence of history of asthma and subjective wheezing: patients with wheezing (n=50), patients with asthma without wheezing (n=45), and patients with both asthma and wheezing (n=20). Increased FeNO level was associated with a history of asthma (odds ratio [OR], 2.47; 95% confidence interval [CI], 1.22–5.02; p=0.012). When subjective wheezing was accompanied by asthma, the OR in patients with increased FeNO was 3.11 (95% CI, 1.23–8.57; p=0.028). These associations persisted after adjustments for age, sex, smoking status, and FEV1 <50% predicted (adjusted OR, 2.96 [95% CI, 1.40–6.29]; p=0.005 for a history of asthma and adjusted OR, 4.24 [95% CI, 1.37–13.08]; p=0.012 for a history of asthma with wheezing). However, there was no association between increased FeNO level and subjective wheezing alone in patients with COPD (Figure 2). When we used FeNO ≥50 ppb, only a history of asthma without wheezing (OR, 4.87; 95% CI, 1.34–17.67; p=0.016) was associated with FeNO ≥50 ppb (Supplementary Figure S1).

Forest plots for odds ratio (OR) of clinical phenotype according to patient classification based on fractional exhaled nitric oxide (FeNO) value: (A) unadjusted, and (B) adjusted data. Adjusted for age, sex, smoking status and forced expiratory volume in 1 second <50% predicted. COPD: chronic obstructive pulmonary disease; ppb: parts per billion; BA: bronchial asthma; CI: confidence interval; aOR: adjusted OR.
3. Prescription of ICS
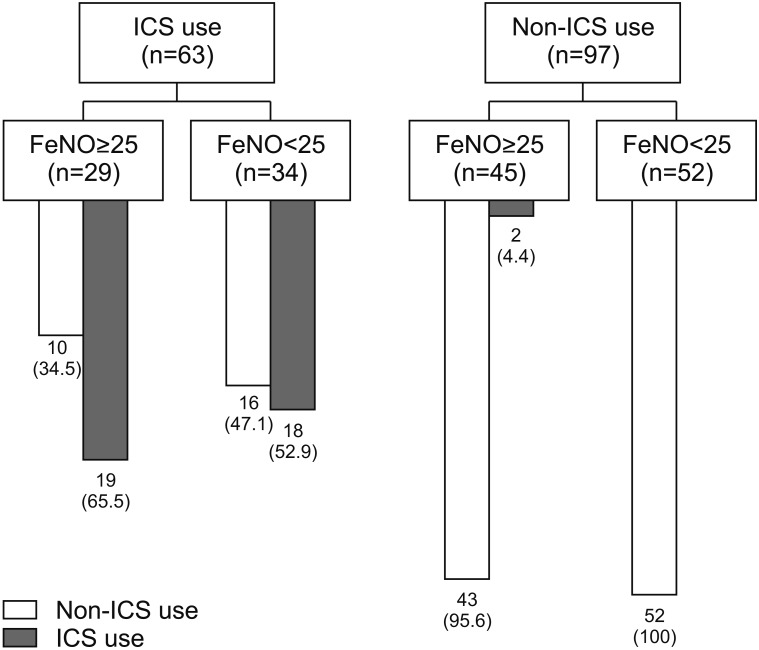
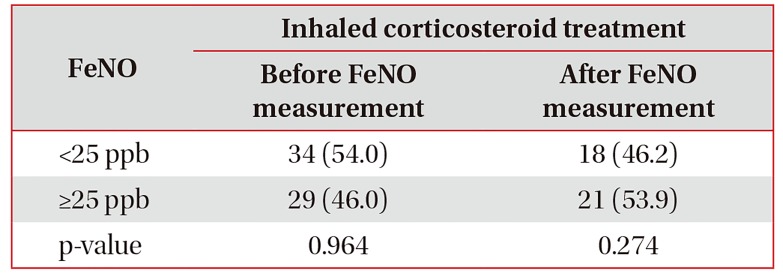
Among 160 COPD patients, 63 used ICS-containing inhalers before FeNO measurement. After FeNO measurement, 39 patients used ICS-containing inhalers and there was no statistical difference between patients with increased FeNO and normal FeNO (21 vs. 18 patients for FeNO ≥25 ppb and <25 ppb, respectively; p=0.274) (Table 3). The pattern of ICS prescription before and after FeNO measurements is shown in Figure 3. After FeNO measurements, only 57% of patients showed concordant prescription (given to increased FeNO group [n=21] and not given to normal FeNO group [n=68]) of ICS-containing inhalers based on FeNO level. Among 63 patients with ICS-containing inhalers before FeNO measurement, ICS-containing inhalers were maintained in 19 patients (65.5%) among those with increased FeNO, while ICS-containing inhalers were withdrawn in 10 patients (34.5%) with increased FeNO. Among 18 patients who maintained ICS-containing inhalers despite of normal FeNO, seven (38.9%) had experienced previous exacerbation before a year of enrollment and two (11.1%) had a history of asthma and wheezing. On the other hand, among 97 patients without ICS-containing inhalers before FeNO measurement, ICS-containing inhalers were newly prescribed in two patients (4.4%) with increased FeNO, whereas 43 patients (95.6%) were maintained non-ICS–containing inhaler despite of their increased FeNO (Figure 3). Among those 43 patients, 42 did not have a previous exacerbation history.

Status of inhaled corticosteroid prescription before and after blood eosinophil and measurement of FeNO levels
Discussion
In this study, we documented a significant association between increased FeNO levels (≥25 ppb) and history of bronchial asthma with or without combined wheezing in a COPD cohort, which persisted even after adjustments for age, sex, smoking status, and FEV1 <50% predicted. Clinicians' prescription decisions regarding ICS-containing inhalers in real-world clinical setting was not significantly differ between normal and increased FeNO groups but it appeared to be affected by clinical presentations such as previous exacerbation and history of asthma with accompanied wheezing.
Based on large-scale clinical trials, current guideline recommends ICS use to be combined with long-acting bronchodilators in patients who experience frequent exacerbations28. In addition, the use of ICS-containing inhalers demonstrated favorable response in terms of reduced exacerbations when the patients exhibited clinical features related to a high Th2-cell signature including history of asthma and had objective parameters indicating eosinophilic airway inflammation2930. However, clinicians in real-world setting often encounter ambiguous history due to recall bias of asthma and uncertain perception of wheezing. Although eosinophils in sputum and blood, as objective indicators for eosinophilic airway inflammation, have been investigated as a promising biomarker to predict the efficacy of ICS1329, various hurdles, including limited accessibility to technicians for sputum eosinophils, and oscillating pattern on repeated testing of blood eosinophils293132, has impeded the use of these biomarkers in daily clinical practice.
One of the alternative parameter reflecting eosinophilic airway inflammation is FeNO. Inducible nitric oxide synthase in the airway epithelium arises due to local inflammation during allergen exposure, leading to significant increase in NO levels33. Accordingly, the utility of FeNO has been highlighted in asthma and partly in COPD with exacerbations. In COPD exacerbations, patients with high FeNO levels at hospital admission are more likely to exhibit a favorable response with regard to lung function recovery at discharge3435. Furthermore, we demonstrated that increased FeNO was independently associated with a history of asthma with or without wheezing, which was consistent with recent studies3637. Thus, the role of FeNO in patients with stable COPD has attracted much attention from clinicians for guidance regarding ICS-containing inhaler therapy. Nevertheless, the clinical application of increased FeNO has not been fully investigated in real-world clinical practice in COPD.
To our knowledge, for the first time, we describe clinical applications of FeNO for the use of ICS-containing inhaler over short periods before and after FeNO measurement. Although ICS-containing inhalers were more frequently prescribed to patients whose FeNO value was increased, it was not clinically significant and FeNO value was not sole indicator to decide use of ICS-containing inhalers for clinicians. When we used FeNO ≥50 ppb, the similar trend was shown for the use of ICS-containing inhalers (Supplementary Figure S2). In other words, the physicians in real-world clinics tended to decide on the use of ICS-containing inhalers based on clinical presentation such as previous exacerbations or previous history of asthma and wheezing in addition to FeNO value. In particular, among those 43 patients, who maintained to use non-ICS–containing inhalers despite of their increased FeNO level, 42 patients did not have a previous exacerbation history. On the other hand, among 18 patients who maintained ICS-containing inhaler despite of normal FeNO, seven patients went through exacerbation and two had asthma history and accompanied wheezing. Those two patients who newly prescribed ICS-containing inhaler, had no previous exacerbation and one patients has asthma and wheezing, but their FeNO level was high. Thus, an integrated approach with clinical features including exacerbation history and suggestive of Th2 inflammation and level of FeNO is applied to clinical decision on the use of ICS-containing inhalers in real-world clinics.
There are several important limitations of the present study. First, FeNO level was measured using two NO analyzers—NIOX MINO and NO breath—depending on the availability. However, diagnostic concordance between the two devices has been reported to be sufficiently high for clinical use38. Second, current smoking status and ICS use are known factors that could affect the level of FeNO39. Because this was an observational cohort study of COPD and small number of each subgroup did not allow us to draw significant conclusion due to insufficient statistical power, we included all patients, regardless of their smoking status (i.e., current smoker) and current ICS users. Third, there was a considerable number of patients who exhibited increased FeNO levels in our study compared with previous studies3436. Because there were no criteria to measure FeNO in patients with COPD in the cohort, and measurement of FeNO was at the discretion of the treating respiratory specialist, there may have been potential selection bias. Finally, because we observed the clinical applications of FeNO over short periods and the effect of FeNO measurements on ICS prescription changes is ambiguous, further studies are needed to investigate the impact of FeNO level on clinical decisions of whether the use of ICS-containing inhalers or not and on future exacerbations over longer-term periods.
In conclusion, increased FeNO is significantly associated with clinical features representing type 2 inflammation. However, clinicians in real-world clinics appeared to regard FeNO as having a subsidiary role in the use of ICS-containing inhalers. Future studies are required to investigate long-term outcome based on level of FeNO, clinical presentations and use of ICS-containing inhalers, thereby assist in identifying ICS responders.
Notes
Authors' Contributions:
Conceptualization: Park HY, Park YB.
Methodology: Jo YS, Park HY, Park YB.
Formal analysis: Jo YS.
Data curation: Jo YS, Choe J.
Investigation: Jo YS, Choe J, Shin SH, Koo HK, Lee WY, Kim YI, Ra SW, Yoo KH, Jung KS, Park HY, Park YB.
Writing - original draft preparation: Jo YS.
Writing - review and editing: Jo YS, Park HY, Park YB.
Approval of final manuscript: all authors.
Conflicts of Interest: No potential conflict of interest relevant to this article was reported.
Funding: No funding to declare.
References
Supplementary Material
Supplementary material can be found in the journal homepage (http://www.e-trd.org).
Supplementary Figure S1
Forest plots for odds ratio of clinical phenotype by patient classification according to FeNO value of 50 ppb.
Supplementary Figure S2
Changes in prescription status of inhaled corticosteroid (ICS) before and after measurement of fractional exhaled nitric oxide (FeNO) levels by FeNO value of 50 ppb.